Are you experiencing pain in the area below your belly button and between your hips for about 6 months or more? Then you must be having chronic pelvic pain. This type of pain can either be a condition of its own or can be a symptom of another disease. It is important that early medical assistance is provided for early diagnoses and better treatment.
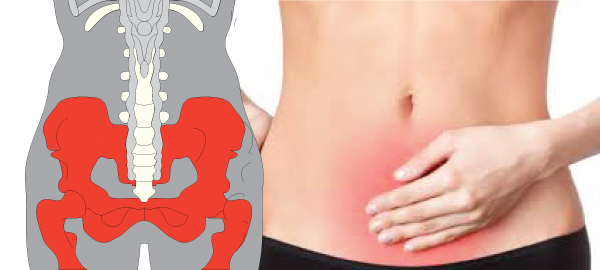
What Causes Chronic Pelvic Pain?
Female pelvic pain is a type of pain below the belly button. It is considered to be chronic if the pain has last for 6 months or more as discussed above. The severity of pain varies per woman, for some it’s a mild pain that eventually goes away, while others feel an intense and steady pain which makes it hard for them to work, sleep or enjoy life.
It is important that the cause of pain is determined to provide proper treatment to the pain. Below are some of the common causes.
1. Endometriosis
This condition is brought about when tissue from your womb’s lining grows outside of your uterus. These mass of tissue thickens, breaks down and bleeds each month as the level of your hormones rises and falls. Because of this, tissues and blood stay in your abdomen, which can lead to fibrous bands of scar tissue or painful cysts.
Signs and symptoms of this problem may include:
- Cramps or pelvic pain before or during your menstruation
- Painful bowel movements and urination
- Painful intercourse
- Pain in the lower back area
- Spotting and rectal bleeding during your periods
- Abdominal bloating
2. Musculoskeletal problems
These are pain or injuries in the human musculoskeletal system including ligaments, joints, nerves, muscles, tendons and structures that support your neck, limbs and back. Musculoskeletal problems such as pelvic floor muscle tension, fibromyalgia or hernia can lead to chronic pelvic pain.
People with this condition often complain body ache, with muscles feel like they have been overworked. Others also experience twitching or burning of muscles, fatigue and sleep problems.
3. Adenomyosis
This condition is similar to endometriosis where cells invade the muscle tissue of your uterus wall.
Though many women with this condition don’t feel any symptoms, other complains heavy periods, menstrual pain, feeling of pressure on the rectum or bladder, spotting between periods and periods that last longer than usual.
4. Interstitial Cystitis
Also known as the bladder pain syndrome or painful bladder syndrome, this is a type of chronic pain that has the presence of bladder pain or pressure, pelvic pain, and urinary urgency or frequency. Women aged 30 and 40 have higher risk of getting this condition. Other symptoms include pain and discomfort when urinating or during sexual intercourse.
5. Urinary Tract Infection
A type of infection, this is often caused by bacteria which involves any part of your urinary tract, including bladder, kidney and urethra. Women are more prone with UTI than men.
Symptoms of this infection include:
- A burning sensation accompanied with pain when you urinate
- Pressure in the lower pelvis
- Frequent urge to urinate
- Cloudy urine, sometimes with the presence of blood
- Lower back pain
- Urine that has bad or strong smell
6. Pelvic Inflammatory Disease
This is an infection of the fallopian tubes, uterus or ovaries that causes them to be infected and inflamed. The infection leaves scars that may cause chronic pelvic pain. Symptoms you may have are:
- Painful sexual intercourse
- Pelvic or abdominal pain either in a specific area or more widespread
- Vaginal discharge with unusual texture, color or odor
- Frequent need of urination with pain
- Cramps that are severe than usual during menstruation
- Fatigue, nausea and fever
7. Pelvic Congestion Syndrome
This is similar to the varicose veins that some women have in their legs, but this syndrome affects the pelvis veins. Veins in the pelvis are engorged and enlarged due to the bloods that are blocked.
You may be experiencing the following symptoms:
- Pain in the pelvic area that gets worse when you stand or sit down
- Pain that begins 7-10 days prior to your menstruation cycle
- Pelvic pain is relieved when you lie down
- Aches in the legs and lower back
- Pain during sexual intercourse
8. Irritable Bowel Syndrome
This is a chronic gastrointestinal & functional bowel disorder which causes abdominal pain, diarrhea, gas, cramps and bloating. Other symptoms are constipation, flatulence, incontinence and pain that is relieved after you have moved your bowel.
9. Pelvic Support Problems
This condition occurs when the ligaments and muscles that hold your organs in place become weak. This results to the organs like the bladder, uterus or rectum to move from their normal location and herniate into your vagina.
Symptoms of this condition includes problem with bowel movements, pain during sexual intercourse, pain in the lower back area, a feeling that something is falling out of your vagina and leak when you’re urinating.
How to Diagnose the Chronic Pelvic Pain
Since many disorders are associated with pelvic pain, diagnosis is needed for proper management. Your doctor will get detailed information about your pain, health history of you and your family. You may be even asked to keep a journal of your pain and other symptoms you’re experiencing.
Examinations that may be suggested by your physician include:
- Pelvic Exam – your doctor will check areas of tenderness to find the signs of infection, tense pelvic floor muscles or abnormal growths.
- Lab tests – your physician may order urinalysis to check if you have UTI or blood test to check your blood cell counts.
- Ultrasound – is used to detect cysts or mass in your ovary, fallopian tubes or uterus.
- Other imaging test – your doctor may request for magnetic resonance imaging(MRI), abdominal X-rays or computerized tomography (CT) scans to check abnormal growths or structure.
How to Treat the Pelvic Pain
The primary goal of the treatment is to reduce the symptoms experienced by the patients and improve their overall quality of life.
Medications such as pain reliever, hormone treatments, antibiotics and antidepressants are prescribed. Doctors may also suggest therapies such as physical therapy, Neurostimulation (spinal cord stimulation), Trigger point injections and Psychotherapy to deal with the pain and other accompanied symptoms of the condition.
A surgical procedure such as Hysterectomy or Laparoscopic surgery may be suggested to correct the underlying problem of the condition. Based on the underlying cause, your doctor will provide the best one for your condition.
